Clinical research blog
Explore our blog for insights into the big questions in precision medicine and clinical research.
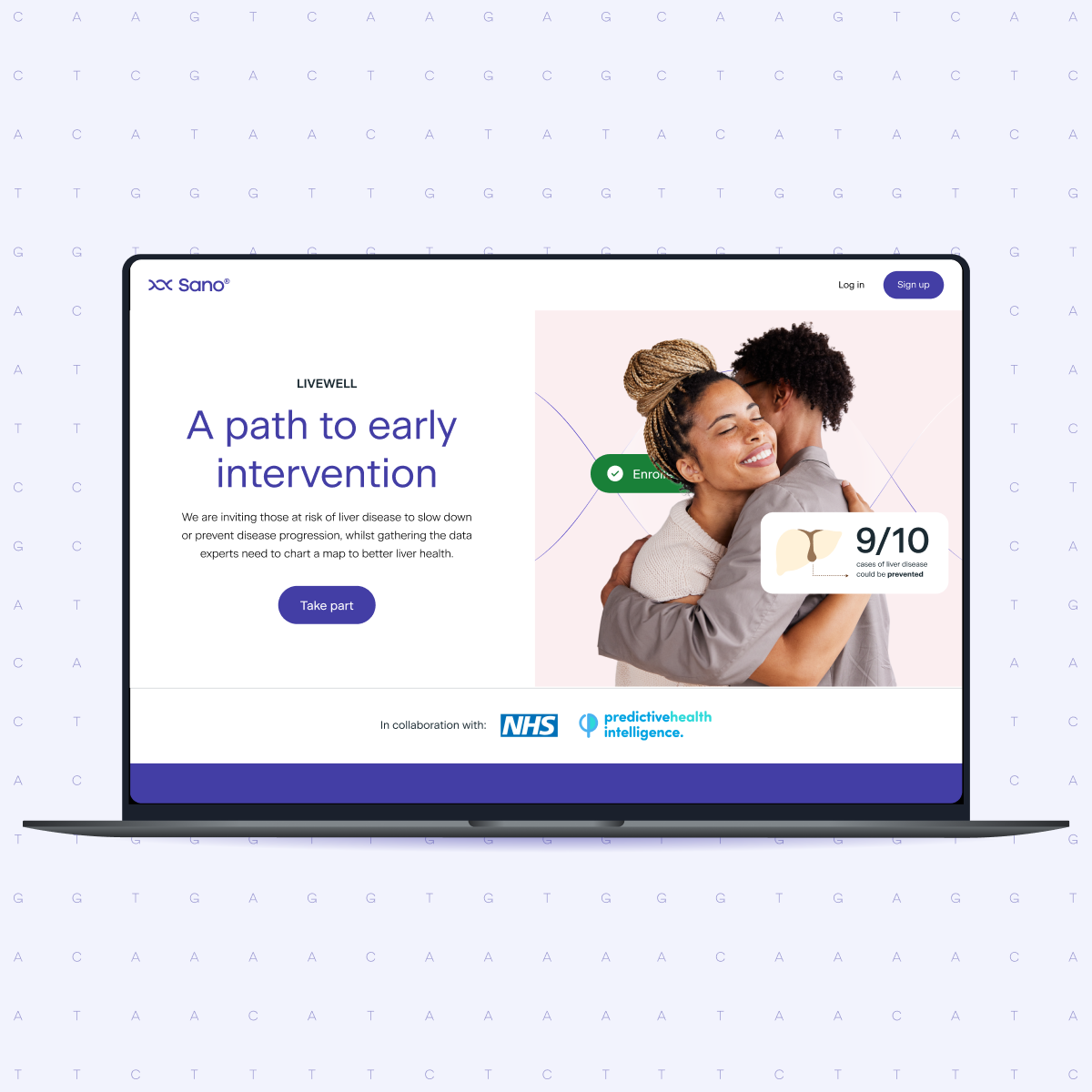
Finding patients who qualify for a clinical trial has always been one of the hardest parts of running one. In liver disease, particularly MASLD, it is especially challenging. With more than 130 active studies competing for the same patient population, screen failure rates are high and recruitment timelines are long. Most approaches rely on standard blood tests that were not designed for population-level screening.
More than three decades after the Huntington's disease gene was cloned in 1993, there is still no approved therapy that alters the course of the disease. Recent high-profile setbacks have underscored a difficult reality: silencing or lowering the mutant huntingtin protein may not be enough. The underlying genetic instability that drives disease progression remains unaddressed.
When a clinical trial misses its enrollment targets, the instinct is often to look at recruitment through more channels, more outreach, and a bigger advertising budget. That response can be useful when the funnel is working as intended. In genetically stratified rare disease trials, however, enrollment pressure is often shaped by decisions made much earlier, including protocol design, access to genetic confirmation, site workflows, consent experience, and the participant journey.
In the most recent episode of The Genetics Podcast, host Patrick Short speaks with Dr. Paul Valdmanis, Associate Professor at the University of Washington, about how long-read sequencing is changing what researchers can see in the genome, and what that could mean for Alzheimer’s disease, ALS, and future neurodegenerative disease therapies.
What four episodes of The Genetics Podcast reveal about the future of Alzheimer’s precision medicine
Alzheimer’s research is entering a new phase. For decades, the field has been shaped by the biology of amyloid plaques and tau tangles. Those remain central to how Alzheimer’s disease is defined and understood.
In the most recent episode of The Genetics Podcast, Patrick Short speaks with Dr. Sarah Marzi, Senior Lecturer at King’s College London and Group Leader at the UK Dementia Research Institute (UKDRI), about ahow genetic and environmental risk factors influence neurodegenerative disease.
Precision medicine sponsors invest heavily to identify, educate, screen, consent, genotype, and support rare patients. In many programs, once a trial ends, that infrastructure does not persist. Patient relationships become inactive, data remains fragmented across systems, and subsequent programs rebuild from the beginning.
UK Biobank and similar resources have made an extraordinary contribution to biomedical research, enabling important advances across genomics, population health, and disease understanding. Recent reports concerning data access have prompted important discussion across the research ecosystem – not about one institution alone, but about how participant trust is maintained as precision medicine becomes more data-intensive, distributed, and global.
Recruitment in precision medicine and rare disease trials remains constrained by fragmented data, low prevalence populations, and heavy reliance on site-based pathways. Even in well-designed studies, a significant proportion of eligible patients are never identified.
On the latest episode of The Genetics Podcast, Patrick Short speaks with Dr. Suzanne Schindler associate professor of neurology at Washington University in St. Louis, about how Alzheimer’s disease develops, why biomarkers like p-tau217 matter, and what new blood-based tools could mean for diagnosis, prognosis, and clinical trials.