Key Takeaways
- Bridging the Gap: Genetic counsellors translate complex genomic data into actionable healthcare decisions for patients.
- Precision Medicine Growth: As the cost of DNA sequencing drops, genetic data is replacing "one size fits all" treatments with tailored medical interventions.
- Informed Consent: Counselors ensure patients understand the risks and benefits of testing, preventing misinformation and unnecessary costs.
- Research Integrity: By building trust and maintaining ethical standards, genetic counsellors increase patient engagement and data quality in clinical trials.
- Access Barriers: Expanding access requires addressing the shortage of qualified professionals and navigating reimbursement challenges like the US CMS recognition.
The rise of precision medicine research
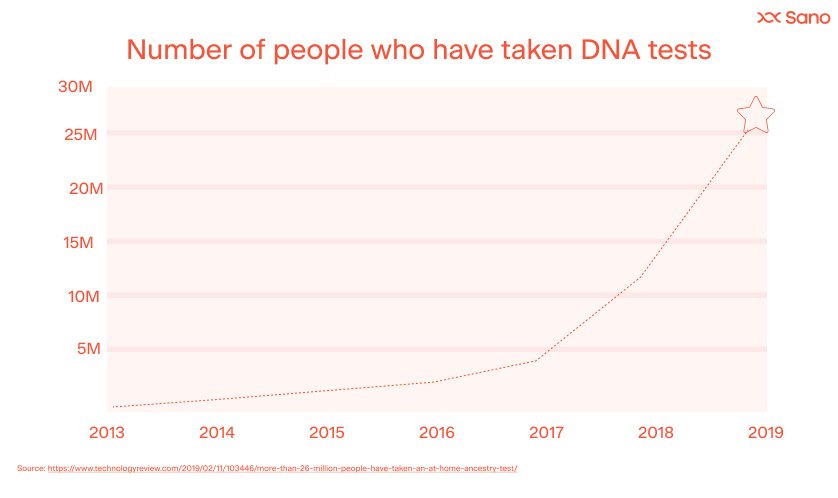
The advent of high-throughput DNA sequencing technologies has made genetic testing faster, cheaper, and more accessible, enabling individuals to access genetic testing directly and contributing to the growth of direct-to-consumer genetic testing services. The below graphs illustrate these advances – the cost per human genome has gone from $100M+ in 2001 to under $1,000 in 2021. And, the number of people who have had their DNA sequenced has risen exponentially. 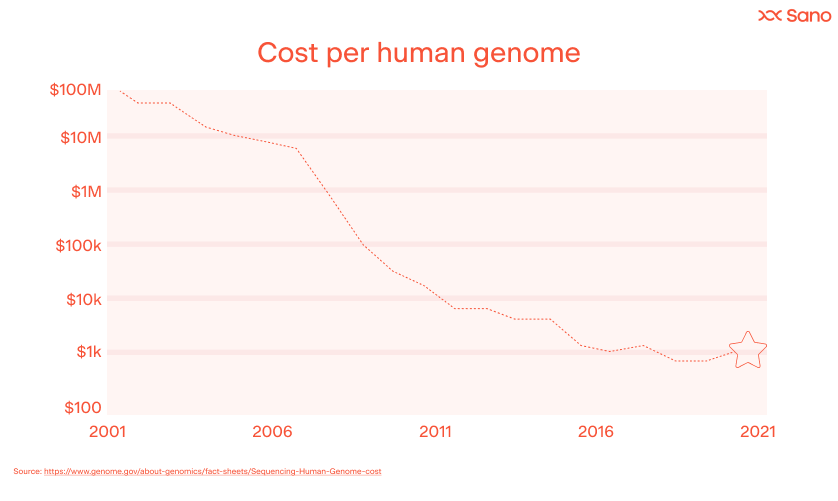
Precision medicine uses this genetic data to move beyond population-averaged treatment models. Rather than prescribing therapies based on broad clinical categories, precision medicine tailors medical decisions and interventions to each individual by leveraging patient-level genetic information to select the most appropriate treatments, therapies, and preventive measures. For sponsors and clinical teams, this shift means that genetic data is no longer supplementary. It is often the primary determinant of eligibility, treatment selection, and outcome measurement. A real-world example can be seen in the antidepressant drug amitriptyline, which is influenced by two genes called CYP2D6 and CYP2C19. Both of these genes affect how quickly the body breaks down amitriptyline. A healthcare provider may therefore use pharmacogenomics to adjust dosage depending on the DNA of their patient to minimise adverse reactions and to make sure the drug is as effective as possible.
As sequencing becomes more integrated into clinical workflows and trial design, the volume and complexity of genetic information patients encounter will continue to grow. This makes the role of genetic counseling more operationally significant, not less.
The role of genetic counseling in precision medicine
Genetic counseling is a vital part of integrating genetic data into healthcare. It encompasses several key functions:
1. Providing educational support and emotional guidance
Genetic counselors assist patients undergoing genetic testing by providing both educational support and emotional guidance. Their work includes gathering and analyzing family history, identifying inheritance patterns, and calculating chances of recurrence for genetic conditions. They are specifically trained to present complex and difficult-to-comprehend information about genetic risks, testing, and diagnosis in terms patients can act on. They offer emotional support and educational resources, helping patients understand their results and prepare for potential outcomes. This support matters when testing reveals risk factors for hereditary disorders, unexpected findings, or results that carry implications for family members.
2. Facilitating informed consent
Genetic counselors play a critical role in ensuring patients fully understand genetic testing's implications. They guide individuals through the complexities, explaining the benefits, risks, and limitations to support informed decision-making.
In precision medicine trials, this is particularly important. Consent involves more than agreeing to participate in a study. Patients must understand why genetic testing is required, how their genetic data will be stored and used, what incidental findings may arise, and what the results could mean for family members. The CDC notes that genetic counseling can help individuals and their families understand genetics and make informed decisions. When counselors address these dimensions clearly, sponsors benefit from higher-quality consent, fewer downstream withdrawals, and more defensible ethical processes.
3. Simplifying complex information
A key function of genetic counselors in precision medicine is to make complex genetic information accessible. This goes beyond translating scientific terminology. Counselors help patients understand the significance of genetic conditions in relation to cultural, personal, and familial contexts. They also discuss available options and can provide referrals to educational services, advocacy and support groups, other health professionals, and community or state services.
In a trial setting, this means counselors can address concerns that extend beyond the study itself, such as implications for family members, insurance considerations, or long-term health management. As genomics becomes more embedded in healthcare and research, this role becomes increasingly important for both providers and patients, ensuring appropriate testing and support while prioritizing patient understanding.
Empowering patients through genetic counseling
Genetic counseling empowers patients to make informed decisions about their care and, in a research context, about their participation in clinical studies. This is especially important as direct-to-consumer genetic testing grows more common and patients encounter genetic information through multiple channels.
In practice, the counseling process typically involves an initial consultation and a follow-up visit for those who undergo genetic testing. During the initial session, counselors review medical history, family history, and draw a family tree to assess hereditary risk. Counselors help patients by:
- Reviewing genetic information and its implications.
- Exploring the psychosocial aspects of genetic data.
- Recommending appropriate screenings or treatments.
- Collaborating with healthcare providers.
This approach enables patients to actively participate in their care, making informed decisions about treatment plans and research involvement. Genetic counseling also provides a layer of psychological support, creating space for patients to process emotions and concerns related to their genetic information. In trial settings, this support directly influences whether patients proceed with testing, consent to participation, and remain engaged over time.
How genetic counseling builds trust and improves research outcomes
Genetic counseling services are pivotal in building trust among patients, researchers, and healthcare providers, leading to a more informed and engaged patient community. This trust, anchored in clear and transparent communication, is crucial for enhancing the quality of research outcomes, ensuring data integrity, and maintaining the ethical standards of the research process. Key contributions of genetic counselors include:
1. Establishing trust with transparent communication
Genetic counselors function as intermediaries between complex scientific processes and patient understanding. By translating genetic information into clear, accessible language, they reduce uncertainty and build confidence in the testing process. This clarity fosters trust not only with patients but also among healthcare providers and research teams. In clinical trials, this trust is directly operational. It influences consent rates, willingness to provide samples, and the quality of ongoing engagement.
2. Improving patient engagement and study participation
Informed patients are more likely to be proactive in research initiatives. Through genetic counseling, patients gain a thorough understanding of genetic testing, personalized treatment options, and the significance of their genetic data in research contexts. This empowerment leads to increased patient participation and commitment to research projects.
3. Enhancing research outcomes
When patients are better informed about why genetic testing is required and what their results mean, conversion through the screening funnel improves. This has a direct impact on enrollment timelines, reduces the cost associated with repeated outreach, and increases the quality of the consented, genetically confirmed population available for study participation. For sponsors running multiple genetically stratified programmes, this effect compounds: participants who engage meaningfully once are also more accessible for future recontact across successive trials.
4. Upholding ethical standards in research
Genetic counselors provide a consistent, patient-centred perspective within trial teams where clinical, operational, regulatory, and commercial priorities must all be balanced. Their role ensures that participants have access to clear, accurate information about testing — independent of the urgency to meet enrollment milestones — which in turn supports the quality of informed consent and the integrity of the data collected. This unbiased approach ensures that patients receive accurate information and guidance, enabling them to make decisions that truly reflect their best interests. Simultaneously, it helps uphold the highest ethical standards in research.
Genetic counseling is integral to fostering a trustworthy, informed, and ethically sound healthcare environment, significantly benefiting both research outcomes and patient welfare.
Challenges in expanding access to genetic counseling
Genetic counseling is essential for patients and healthcare providers, but its widespread availability faces challenges. Key among these is the limited number of genetic counselors, a factor that restricts access to expert genetic advice in the United States, the United Kingdom, Europe, and other regions.
Addressing the shortage of genetic counselors
The scarcity of genetic counselors creates a bottleneck in delivering genetic services at scale. For sponsors running multi-site or multi-country trials, this shortage affects site capability, geographic coverage, and the consistency of patient communication. Counselors are not only patient-facing. They also serve as a central resource of information about genetic conditions for other healthcare professionals, which means their absence affects the broader study team.
Training programs and certification initiatives are expanding to address this gap, but demand continues to outpace supply. For sponsors, this underscores the importance of planning counseling capacity early in study design rather than assuming availability at the point of need.
Reimbursement barriers for genetic counselors in the US
In the United States, a significant hurdle is that the Centers for Medicare and Medicaid Services (CMS) has historically not recognized genetic counselors as healthcare providers. This limitation restricts the availability of genetic counseling for many people. Legislative efforts, including the Access to Genetic Counselor Services Act, have sought to address this gap. Progress on provider recognition remains a key factor in determining how broadly genetic counseling services can be accessed across the US healthcare system.
Expanding access through remote genetic counseling
To overcome geographical barriers, remote genetic counseling services, including video-based and telephone-based models, are becoming more widely adopted. These services allow individuals in rural or remote areas to access expert genetic counseling without requiring an in-person visit.
For clinical trials, remote counseling is particularly relevant. It reduces site burden, supports decentralized study designs, and enables sponsors to reach geographically dispersed patient populations more consistently. It is also worth noting that genetic testing is not a required part of the genetic counseling process. Patients can gain valuable information from a counseling session without proceeding to testing, which means counseling can serve as an independent engagement and education step within the trial workflow.
Industry collaboration to expand genetic counseling access
For sponsors running genetically stratified trials, the limited availability of genetic counselors is not only a healthcare access issue — it is an operational constraint. When counseling capacity cannot scale with screening volumes, participant drop-off at the testing stage increases, enrollment timelines lengthen, and the cost of qualifying each participant rises. Integrating scalable counseling support — including remote and digital delivery models — directly into trial workflows allows sponsors to mitigate this bottleneck without depending on healthcare systems to resolve it independently.
The shortage of qualified genetic counselors remains a structural constraint on precision trial execution. Without coordinated investment from sponsors, CROs, and healthcare institutions in expanding counseling capacity and remote delivery models, access limitations will continue to constrain the depth and representativeness of genetically stratified cohorts.
Conclusion
Genetic counseling is not a peripheral service in precision medicine. It is a structural component that influences consent rates, testing completion, data quality, participant trust, and long-term engagement. For sponsors running genetically stratified trials, the availability and quality of genetic counseling directly affects how many patients can be evaluated, enrolled, and retained.
As more therapies target specific genetic variants, the demand for integrated counseling workflows will continue to grow. Sponsors who build counseling into their study design from the outset, rather than treating it as an afterthought, will be better positioned to execute effectively and maintain ethical standards across their programs.
To learn more about how Sano integrates genetic testing and counseling into precision medicine workflows, get in touch.


