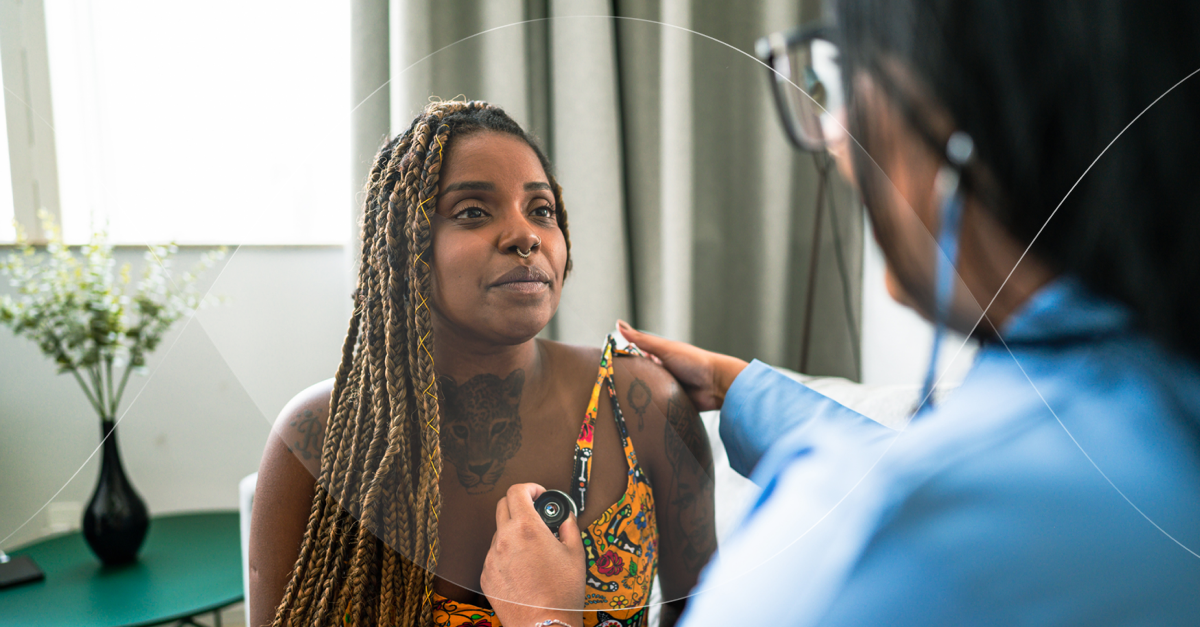Meaningful diversity means that trial participants match the disease burden within a given geography. This includes representation across race, ethnicity, age, gender, socioeconomic background, and geography. And recently, we've seen growing recognition of the importance of inclusivity and representation in clinical research, driven by both scientific necessity and increasing regulatory expectations. Below, we outline practical steps that sponsors and research teams can take to address the problem.
Key Takeaways
- Address the Representation Gap: Current clinical trials are 76% white, failing to reflect global demographics where 60% of the population is in Asia and 16% in Africa.
- Build Community Trust: Partner with local organizations and leaders to overcome historical skepticism and reach underserved groups.
- Reduce Participation Barriers: Simplify consent forms and offer logistical support like transportation, childcare, or virtual trial options.
- Diversify the Workforce: Inclusive research teams help identify cultural biases and foster a more welcoming environment for diverse participants.
- Enhance Communication: Use culturally appropriate materials and patient engagement technology to improve retention and satisfaction.
Raise awareness and education
Low awareness of clinical research opportunities is not evenly distributed. It is concentrated in communities that have historically been excluded from, or harmed by, medical research. This is a structural issue, not simply an information deficit.
Many people are not aware of their value in medical research or of the importance of the research in general. Others live in communities that have been directly impacted by historical harms related to clinical research, and have developed justified skepticism of the medical system. Addressing this requires more than broad outreach. It requires targeted campaigns, social media, and community engagement designed to reach specific populations with relevant, culturally appropriate information.
Patient-facing healthcare professionals also play an important role in raising awareness of research opportunities within communities of color. Educating researchers about the benefits of diversity and the potential biases that can arise from homogeneous trial populations is equally important. When research teams understand how representation gaps affect data quality and regulatory outcomes, the case for change becomes operational, not just aspirational.
Collaborate with community organizations
Engaging with community organizations addresses one of the deepest barriers to diverse enrollment: trust. Many potential participants carry justified concerns rooted in mistrust of the healthcare system, stigma, lack of access to information, and fear. Community organizations have the relationships and credibility needed to bridge that gap.
These groups can help draw attention to clinical trials, address concerns or misconceptions, and reach participants from underserved groups. Working alongside these organizations and fostering relationships with trusted leaders enables researchers to connect with diverse participants and build ongoing communication and recruitment pathways that persist beyond a single study.
Simplify trial procedures
Complex trial procedures and overly restrictive eligibility criteria disproportionately exclude underrepresented groups. This makes protocol design itself a lever for improving diversity.
At the protocol level, sponsors can review inclusion and exclusion criteria for requirements that inadvertently narrow the eligible population without clear scientific justification. Criteria based on prior treatment history, comorbidity thresholds, or geographic proximity to specific site types can systematically exclude patients from underserved communities. Inclusive protocol design means evaluating these criteria with diversity outcomes in mind from the earliest stages of study planning.
At the operational level, research teams can simplify consent forms, offer translation assistance, provide transportation or childcare support, and consider flexible scheduling. In some cases, clinical trials could be virtual rather than in-person, which removes difficult barriers to participation for many. Together, these design and procedural changes open clinical trials to a wider participant range.
Improve cultural competence
Cultural competence means understanding and respecting the cultural backgrounds and values of diverse populations. Clinical trials should be designed and conducted in a culturally sensitive way. This means asking for diverse opinions and perspectives on study design and involving community leaders or advocates from underrepresented groups in the research process. Trial materials must also be culturally appropriate and accessible whenever possible.
Building this competence requires more than intent. It requires structured training for both internal teams and external partners, focused on health equity, unconscious bias, and inclusive communication. When training is embedded into study operations rather than treated as a one-time exercise, it creates consistency across sites and geographies.
Cultural competence builds trust with participants from diverse backgrounds, which supports consistent engagement and reduces dropout rates — both of which contribute to more complete and representative data.
Diversify research teams
Diverse research teams bring perspectives and insights that help identify potential biases or barriers to participation. Actively seeking diversity in research teams creates an environment of trust and understanding, which often paves the way to engaging trial participants from different backgrounds. Some organizations are making this a priority. For example, the Association of Clinical Research Professionals (ACRP) formed a Diversity Advisory Council, a working group dedicated to reinforcing the need for "greater diversity in the clinical trial workforce."
Equally important is site and investigator selection. The geographic and institutional placement of trial sites determines which patient populations have realistic access to participation. Selecting sites in communities with higher concentrations of underrepresented groups, and choosing investigators who reflect or have established relationships with those communities, is a direct and measurable way to improve enrollment diversity.
Enhance participant engagement and communication
Engagement and communication directly influence which participants stay in a trial and which drop out. When communication is unclear, inaccessible, or culturally misaligned, the result is differential attrition that erodes diversity over the course of a study. Clear and concise communication from researchers about the purpose, benefits, and risks of the trial is essential.
To promote inclusivity, researchers should think about tailoring communication materials to make them more inclusive, as well as using language that is easily understood and offering language assistance where needed. Innovative patient engagement technology can support clinical trial patient retention. Actively involving participants in the trial process, providing regular updates, and seeking feedback helps participants feel valued and improves overall engagement and satisfaction.
None of this works without continuous measurement. Sponsors should track diversity metrics at each stage of the funnel, from awareness through enrollment and retention, and use that data to adjust strategies in real time. Without performance visibility, diversity commitments remain aspirational rather than operational.
Build partnerships across the research ecosystem
Advancing diversity in clinical trials requires coordination across researchers, policymakers, healthcare providers, patient advocacy groups, and sponsors. No single organization can address the full range of barriers independently.
Sometimes this is achieved via steering committees or advisory boards with members from different stakeholder groups. Working together, stakeholders can share best practices, develop guidelines, and implement policies that promote diversity and inclusivity. This can also help address systemic barriers and create a supportive network for diverse clinical trial participation.
Importantly, diversity is a global challenge that requires locally tailored strategies. What works in one geography may not translate to another. Effective collaboration means developing regional approaches informed by local regulatory requirements, cultural contexts, and patient population characteristics, rather than applying a single framework across all markets.
Final thoughts
Improving diversity in clinical trials is not a single initiative. It is an operational discipline that spans protocol design, site selection, community engagement, participant communication, and ongoing measurement. Each of these areas requires deliberate planning and sustained execution across the full study lifecycle.
For sponsors running precision medicine programs, these challenges are amplified. Genetically stratified trials, rare disease studies, and multi-country programs require reaching specific populations across geographies, often with additional complexity around genetic testing, counseling, and long-term engagement. Diversity cannot be addressed as an afterthought in these contexts. It must be built into the recruitment and engagement strategy from the start.
Sano supports sponsors in designing and executing recruitment programs that reach diverse, genetically defined populations across multiple markets. From omni-channel recruitment and at-home genetic testing to long-term participant engagement and recontact, the platform is built to reduce the structural barriers that limit who participates in research. Get in touch to discuss how this applies to your program.